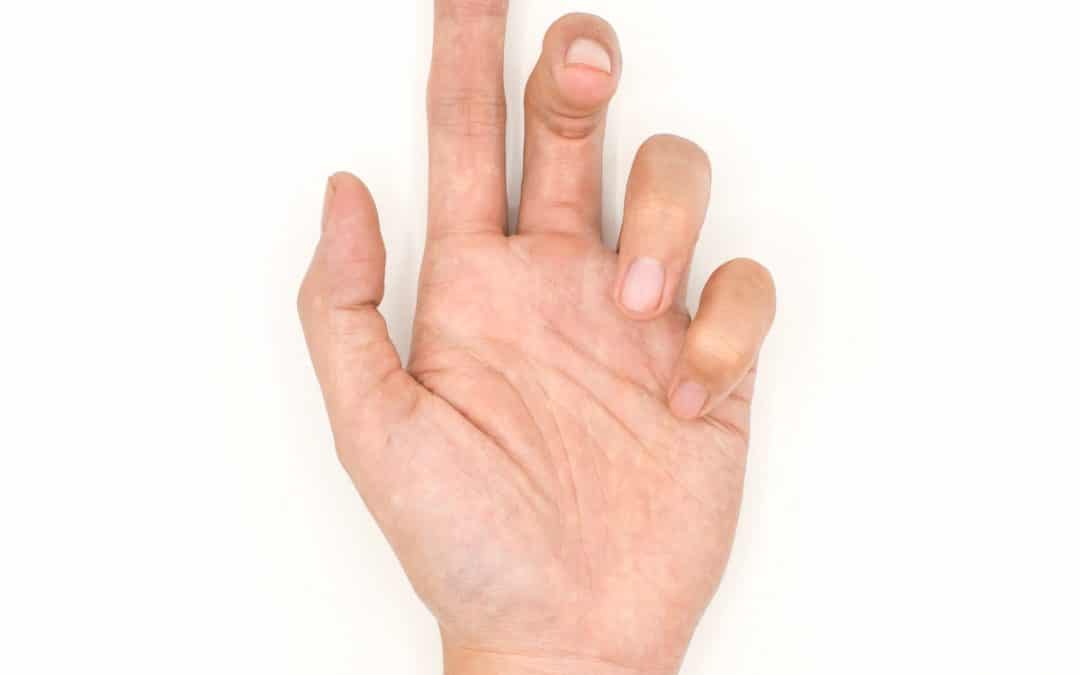
Dupuytren’s Contracture is a condition that affects the connective tissue under your skin. It causes the skin to scar which in return limits movement. The condition causes the fingers to be pulled in towards the palm of the hand, which is often how physicians diagnose it.
What causes the condition is still unknown to doctors, but it is believed to be genetic as it’s seen within families. Other known risk factors include alcohol and tobacco use, epilepsy, and diabetes.
Symptoms
Dupuytren’s Contracture is characterized by the abnormal thickening of tissue under the palm of the hand. The first symptom is often a small lump in the palm, usually near the base of the fingers. The lump(s) may feel tender but are not painful. They also develop over a longer period of time.
Occasionally, patients will experience what are called “knuckle pads.” This is where the skin will thicken on top of the knuckles.
Overtime, a fibrous cord may form in the hand. This is what results in the fingers being pulled inward towards the palm. In the most severe cases, patients will be unable to perform everyday activities such as picking up items or washing their hands.
There are several risk factors which can also contribute to one developing Dupuytren’s Contracture:
- -Gender: Men develop the condition more often than women
- -Heritage: Those of northern European descent (English, Irish, Scottish, French) and Scandinavian descent are predisposed to developing the condition
- -Genetics
- -Frequent alcohol use
- -Old age
- -Diabetes
- -Seizure disorders such as epilepsy
Diagnosis
Physicians can normally diagnose Dupuytren’s Contracture just by looking at and feeling a patient’s hands;other tests are rarely needed.
Tabletop Test
The Tabletop Test is one of the quickest ways for doctors to diagnose Dupuytren’s Contracture. The patient will place their hand on a table, palm down. The doctor will have the patient lay their hand as flat as possible against the table. If they cannot, this is a sign of Dupuytren’s Contracture.
If your hand remains arched, it may be a sign of a severe contracture. There are several options to treat Dupuytren’s Contracture but if it is a severe case, surgery may be the only option.
Non-Surgical Treatments
Radiation Therapy
Radiation therapy has been found to be effective in treating the early stages of Dupuytren’s Contracture. While it cannot reverse any contracture that is already there, it can slow down the progression of the disease.
The radiation is used at a smaller frequency than it is for cancer patients to mitigate side effects. A common side effect may be dryness and irritation of the treated area. Doctors have not found any significant increase in the risk of getting cancer from this kind of treatment either.
Most patients will go through two rounds of RT that consist of five. daily treatments or seven doses over a two week period. It depends on each patient’s needs.
Steroid Injections
Corticosteroids are not guaranteed to relieve symptoms, but they can relieve pain when injected into an inflamed nodule. In certain cases, they can even slow a contracture in the hand.
Enzyme Injections
Enzyme injections are a newer treatment with promising results, although research is still being conducted on the long-term effects. An enzymatic solution containing collagenese is injected directly into the nodules of the hand.
In the 24 to 72 hours following injection, the enzymes weaken and dissolve the affected tissue. Patients may experience reduced pain and increased hand function.
When Do You Need Surgery
Waiting too long to have surgery can result in a failed operation, or needing multiple surgeries. Some patients who wait too long may only regain partial use of their hand and fingers. Open surgery is also more invasive, and comes with a longer recovery period. There are two procedures which are typically used to treat Dupuytren’s Contracture.
Fasciotomy
The fasciotomy is performed under local anesthetic. Your doctor will make a small incision in your palm in order to divide the thickened cords. While the cords are not removed, dividing them releases tension in the palm. This in turn, gives the patient more range of motion in their fingers and alleviates pain.
After the procedure, the wound is left open to heal. Patients will need to wear a splint to prevent damage to the incision site.
Sub-Palmar Fasciotomy
This procedure is more extensive than a fasciotomy and tends to require more physical therapy and longer recovery. The surgeon can use a variety of incisions but will normally opt for a “zig-zag” along the natural creases of the hand.
From there, the surgeon will remove as much abnormal tissue and cord as possible to allow the fingers to straighten again. Depending on the severity of the condition, your wound will either be left open to heal or will require a skin graft. Patients may also have to wear a splint during their recovery.
Risks
The risk associated with the above procedures depends on the severity of the contractures and the patient’s medical history. Your surgeon will discuss the risk associated with each procedure prior to surgery which may include:
- -Scarring
- -Nerve damage
- -Infection if the wound isn’t properly cared for
- -Stiffness
- -Loss of sensation (sometimes temporarily)
Pain, swelling, and stiffness are common during recovery. While the goal isn’t to cure but improve hand-function, some patients may require additional surgeries to achieve maximum results.
Once you’re cleared, you may be recommended to a physical therapist in order to increase hand strength. This will prevent stiffness and help you regain muscle strength.
Percutaneous Aponeurotomy
A newer surgery method called a percutaneous aponeurotomy also known as “needling” is a fairly new treatment, but has better benefits. Dr. Brutus is one of few surgeons in Canada who can perform this surgery. He has seen a 95% success rate in his patients.
Depending on where the fibrous cords are in your hand, age, family history, and severity, needling may be a viable treatment option.
The procedure is performed as an outpatient procedure under a local anesthetic. This treatment is less invasive, allowing patients to resume daily activities sooner. This procedure is beneficial because it does not require incisions, post-operative care, physical therapy, and has little to no down time. Aponeurotomy can easily be repeated in cases where symptoms recur.
Final Thoughts
Dupuytren’s Contracture gradually occurs over time, giving you time to slow down its progression. While there is no cure for this condition, being able to ease symptoms and improve hand function will go a long way in improving a patient’s quality of life. Recognizing early signs will be key to preventing permanent loss of hand-function.